Written byAdam Waldbillig
CBD has gained a lot of popularity in recent years due to its health benefits and lack of ‘high feeling’ when administered. This article will explore the formulations, pharmacology, and potential applications for CBD oil and diabetes
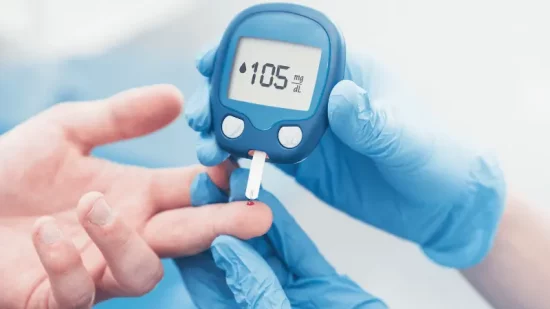
The name diabetes mellitus, ‘diabetes’ being derived from the Greek word ‘siphon’- to pass through and ‘mellitus’ meaning honeyed or sweet, is the result of untreated diabetics having high levels of glucose in the urine. This is a characteristic of diabetes that can be attributed to glucose not being absorbed by the body’s tissues due to a complete or partial lack of insulin.
More recently, Cannabis has started to enter the conversation due to its broad pharmacological spectrum of action, and more specifically, its potential as a viable immunosuppressant.
Two Types of Diabetes
Diabetes can then be divided into 2 distinct groups: type 1 diabetes (T1DM) and type 2 diabetes (T2DM). Individuals with this disease can manage their illness with medication, exercise, and diet.
Type One
Type 1 diabetics manage their disease diligently with blood glucose monitoring (BGM), insulin injections, and consistent tracking of dietary carbohydrates. Even with good control of blood glucose, the long-term effects of living with this chronic metabolic condition are proliferative retinopathy, nephropathy, cardiovascular disease (CVD), and impaired healing.
Type 1 diabetes is an autoimmune disease that is characterized by the destruction of β-cells in the islets of the pancreas. The result is an absolute deficiency in insulin1 (Zhang, X. F. & Tan, B. K. H, 2000), a peptide hormone that regulates the uptake and storage of glucose.
Type 1 diabetes is likely caused by a genetic predisposition and therefore symptoms are usually detectable in early life (childhood to adolescence) but can be diagnosed at nearly any age. The criteria of fasting hyperglycemia, meaning an elevated blood sugar level after 8 hours without eating, is most common in diagnosing diabetes mellitus. A fasted plasma glucose of ≥126 mg/dl (7.0 mmol/L) or casual plasma glucose of ≥200 mg/dl (11.1 mmol/l) is considered diabetic.
Type Two
Type 2 diabetics also need to consider down the road complications while maintaining a healthy lifestyle. The peer-reviewed scientific literature on Cannabidiol (CBD), the non-psychoactive component of Cannabis, has been effective in treating some of the complications of diabetes in experimental disease models.
Type 2 diabetes is the result of a combination of resistance to insulin action and an inadequate compensatory insulin secretion response1 (Zhang, X. F. & Tan, B. K. H, 2000). Most patients with this form of diabetes are obese or have body fat distributed predominantly in the abdominal region.
Type 2 diabetics may experience a longer onset of the disease in which hyperglycemia remains undetectable and ketoacidosis seldom occurs1 (Zhang, X. F. & Tan, B. K. H, 2000). Even though insulin levels may seem normal or even elevated in these individuals, elevated blood sugar occurs due to their normal β-cell function not being able to accommodate for the insulin resistance3 (Kahn, B. B. & Flier, J. S).
Type 2 diabetics however are not dependent on exogenous insulin for survival and treatment involves a regimen of proper diet and exercise. Type 2 diabetes along with obesity is linked to a wide array of disorders called metabolic syndrome which include hypertension, hyperlipidemia, and low HDL-cholesterol. Type 2 diabetics also have a strong genetic predisposition however the genetics are much more complex than Type 14 (Leiter, E. H, 1989).
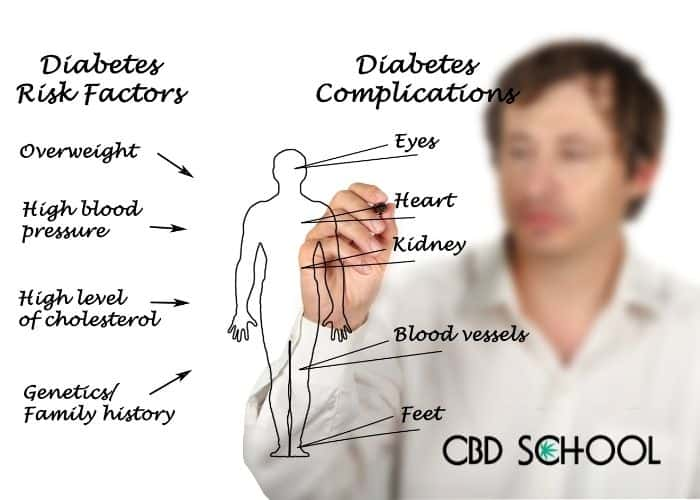
What is Diabetes and What Causes it?
Insulin can be thought of as the ‘key’ which unlocks the cell and allows the passage of glucose, the body’s most essential energy molecule. This form of diabetes is associated with molecular markers such as serum autoantibodies to β-cells of the pancreas, autoantibodies to insulin, autoantibodies to tyrosine phosphatase IA-2 and IA-β2 (Wang, X. et al.).
Other symptoms of high blood glucose include excessive thirst, excessive urination, and blurred vision. This will also likely be accompanied by a state of diabetic ketoacidosis (DKA) in which ketones are detected in the urine. Severe cases of DKA may cause hospitalization and even death.
In terms of numbers, about 35.2 million people have diabetes in the United States with 90-95% of all diabetics being type 2 with most of the rest being type 1 according to the American Diabetes Association.
Diabetes is a metabolic illness that lasts an entire lifetime which in turn causes complications down the road. The most common complications for these individuals are proliferative retinopathy, nephropathy, cardiovascular disease (CVD), and impaired healing5,6 (Nathan, D. M. et al, 2009; Brem, H. & Tomic-canic, M, 2007).
Multiple reviews of the therapeutic potential of CBD have been appraised and published7-12 (Pisanti, S. et al, 2017; Booz, G. W, 2011; Pertwee, R. G, 2008; Laprairie, R. B et al., 2015; Campos et al., 2012; World Health Organization) with an overwhelming amount of evidence for immunomodulation and modulation of neuronal and cardiovascular function. Here the science of CBD is reviewed and research has gone into the specific complications associated with diabetes.
Cannabinoids and Diabetes
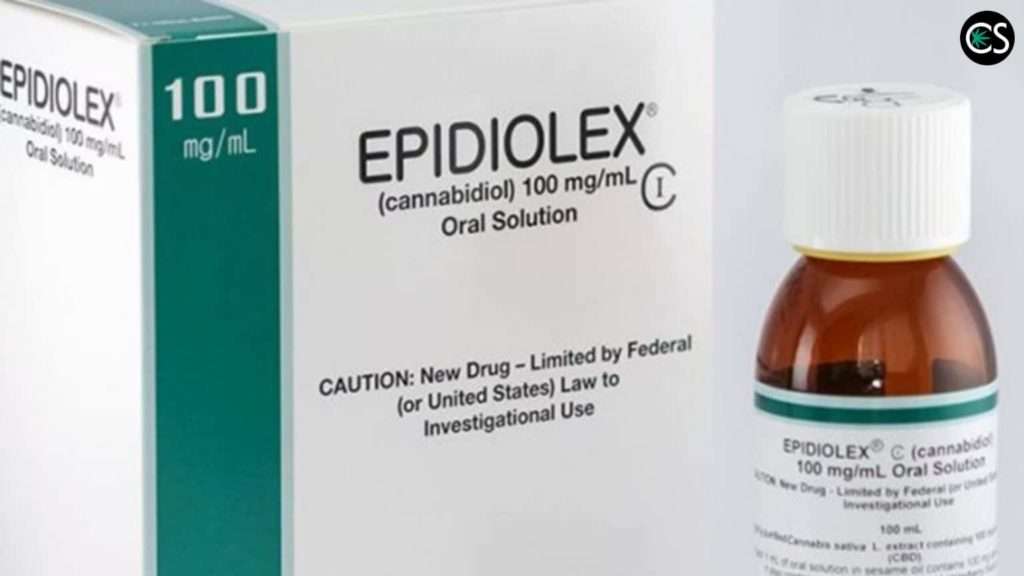
Sativex® and Epidiolex® from GW pharmaceuticals are two pharmaceuticals that have been developed that are a purified form of plant-derived cannabinoids. FDA approval is still pending for Sativex® but Epidiolex® has been approved for the management of seizure intensity and frequency of people with Lennox-Gastaut Syndrome (LGS) and Huntington’s disease.
Epidiolex® is a high purity CBD product and Sativex® is a 1:1 CBD/ THC formulation with a few other minor cannabinoids. Some states and jurisdictions have legalized marijuana in which case products that include THC are very accessible. Since CBD is highly non-toxic or psychoactive, many formulations are available legally which include many CBD products like oils, tinctures, nasal sprays, edibles, topicals, capsules, and flower.
High purity CBD oil has become a viable complementary alternative medicine (CAM) and can be bought without a prescription. Most products are all-natural and plant-derived due to certain plant cultivars having naturally high CBD and low THC content13 (Small, E. & Beckstead, H, 1973).
A tincture is essentially CBD dissolved in ethanol and later incorporated into an oil such as MCT. CBD is fat-soluble and therefore most products appear oily. Tinctures are applied dropwise sublingually (under the tongue) or sprayed orally for the highest % absorption of the bloodstream14,15 (Stott, C. G et al., 2013; Lucas, C. J., 2018).
CBD oil only has 6% bioavailability when ingested meaning the remainder will be metabolized and passed through the digestive system, this means it is important to find a high potency CBD formulation for edibles and capsules.
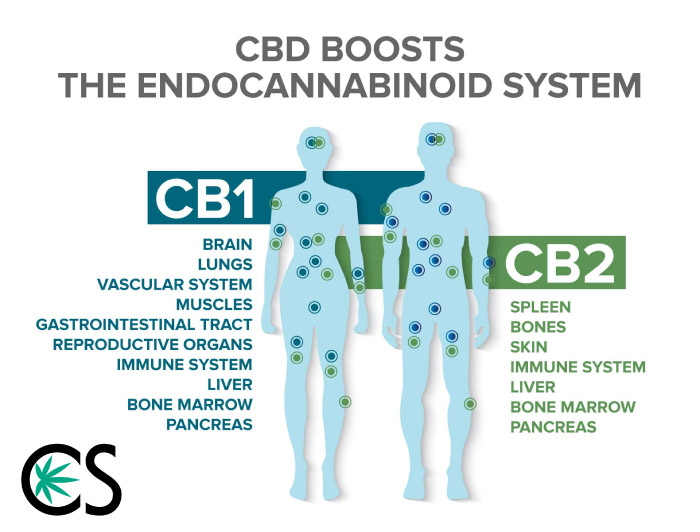
To get into the other effects of CBD oil we need to talk about your own cannabinoids. Your endocannabinoid system consists of anandamide (AEA) and 2-arachidonoylglycerol (2-AG). Phytocannabinoids (naturally occurring THC, CBD, and other cannabinoids found in the cannabis plant) essentially mimic these signaling molecules and bind the same receptors, to a certain degree.
Read: The Endocannabinoid System Explained
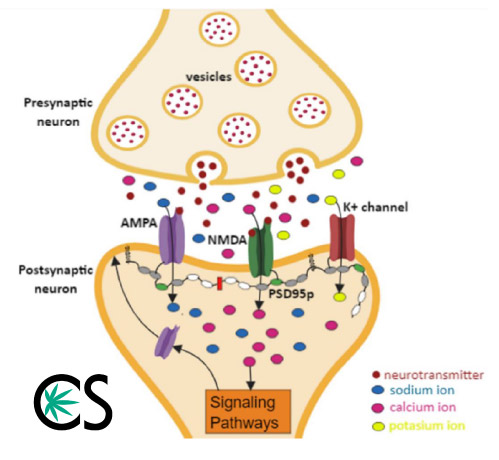
Since THC was discovered first, which later led to the discovery of the endogenous cannabinoid system, everything is named after the Cannabis plant. Endocannabinoids regulate neuronal firing through a process called ‘retrograde synaptic signaling’ where they may inhibit the further release of excitatory neurotransmitters.
Basically, endocannabinoids are made in a response to excitation and ‘pump the breaks’ on further neuronal synapses. A point of contention for many researchers has been to describe what CBD does at cannabinoid receptors (CBs) meaning how well does it bind, where does it bind and what is the result of that receptor being activated.
It may be surprising, however, that CBD does not actually bind cannabinoid receptor 1 or 2 or any receptor with a very high affinity16 (Tham, M. et al., 2019). It does, however, interact with many receptors on different tissues, such as adenosine A2A receptors17 (Castillo, A. et al., 2010) and transient receptor potential channels (TRP)18 (Iannotti, F. A. et al., 2014).
An agonist is something that binds a receptor and elicits the full effect, AEA is a full agonist at cannabinoid receptor type 1 (CB1)19 (Deutsch, D. G. & Chin, S. A., 1993). An antagonist is something that blocks the effects of the agonist, CBD has been described as an antagonist before, but as new research emerges scientist believe it actually doesn’t even bind the active site of the receptor at all, making it an ‘allosteric modulator’ of CB110 (Laprairie, R. B et al., 2015).
Allosteric modulators have great potential as drug candidates because they can modify the effects of endogenous signaling molecules, such as 2-AG and AEA20 (Laprairie, R.B. et al., 2017). This fact helps build the case for CBD oil as a therapeutic.
Inflammation and Immunosuppression
CBD products have been implicated in targeting the immune system and reducing inflammation by action at multiple receptors. The immune system is necessary to heal the body and fight infections, however chronic inflammation and the sustained release of pro-inflammatory cytokines and reactive oxygen species (ROS) becomes problematic over time.
These cytokines consist of primarily TNFα and IL-6 while reactive oxygen species harbor free radicals and can oxidize tissue which leads to further damage21 (El-Remessy, A. B. et al., 2008). THC has been established as a partial agonist of CB1 which is primarily found in the central nervous system22,23 (Hua, T. et al., 2016; Morales, P. et al., 2018) while CBD has a higher affinity for CB2 receptors which are localized on cells of the immune system such as B lymphocytes, microglia, macrophages, mast cells, natural killer cells and the lymphatic organs24 (Navarro, G. et al., 2016).
In most models of inflammation, CBD attenuates inflammatory cell migration and ROS, TNF, p38 MAPK activity8 (Booz, G. W, 2011) which may, in turn, reduce chronic pain and swelling. Chronic pain in the body is a response to prostaglandin (PGE2) production which is synthesized by COX-1 and -2 enzymes25 (Ruhaak, L. R. R. et al., 2011).
A study in which CBD was administered orally (5-40 mg/kg) once a day, 3 days following injection of carrageenan, which causes a PGE2 increase in rats showed that PGE2 production, COX activity, and production of ROS, were all reduced in a dose-dependent fashion26 (Costa, B. et al., 2004).
CBD also had anti-inflammatory effects in a mouse model of acute lung injury. CBD reduced neutrophil migration into the lungs, albumin concentration in bronchoalveolar lavage fluid, myeloperoxidase activity in the lung, and production of TNF and IL-6 with these effects mediated by A2A receptors27 (Ribeiro, A. et al., 2012). Once further, a low concentration of CBD in a mouse stroke model demonstrated a reduction in Il-6, TNF-α, COX-2, and iNOS expression, these effects were mediated by CB2 and Adenosine receptors as well17 (Castillo, A. et al., 2010).
A few very interesting prospective studies have demonstrated that CBD may actually attenuate or delay the onset of Type 1 diabetes in a mouse model. Major effectors of β-cell destruction are various free radicals and oxidant species and inflammatory cytokines8 (Booz, G. W, 2011).
CBD has been reported to significantly reduce insulitis and beta-cell destruction28,29 (Weiss, L. et al., 2006; Weiss, L. et al., 2008) Two studies using a T1DM mouse model of diabetes show that only 32% of CBD treated mice were diagnosed, while 100% developed T1DM in control groups.
CBD treatment suppressed production of Th1 associated cytokines IL-12, IFN-γ, and TNFα suggesting deviation from destructive Th1 immunity to protective Th2 immunity28 (Weiss, L. et al., 2006;).
CBD administration reduced the level of pro-inflammatory cytokine IL-6 and increased the level of anti-inflammatory IL-1029 (Weiss, L. et al., 2008). These results strongly support CBD oil as being clinically anti-inflammatory and effective in reducing the autoimmune response.
Retinopathy
Atherosclerosis, meaning hardening of the blood vessels, is the most common macrovascular complication of diabetes and may contribute to diabetic retinopathy8 (Booz, G. W, 2011). Retinopathy affects 3/4 of all diabetics 15 years post diagnosis30 (Klein, B. E. K. et al., 1991)
Due to increase blood viscosity from chronic hyperglycemia, the tiny thin capillaries of the eye are at risk of damage in TIDM and T2DM31,32 (Trap-Jensen, J. & Lassen, N. A., 1968; Porta, M., 1987). Retinal cell degradation is a common diabetic complication and people with diabetes usually see an eye doctor regularly.
Diabetics also experience Oedema, meaning the accumulation of fluid due to capillary hyperpermeability which may lead to blindness in some cases32 (Porta, M., 1987). Anti-inflammatory experiments performed in rat retinas and retinal microglial cells showed that CBD inhibited TNFα accumulation from LPS-induction (LPS stimulates the immune system)21 (El-Remessy, A. B. et al., 2008).
CBD has also attenuated high-glucose damage to coronary endothelial cells33 (Rajesh, M. et al., 2007). This research is promising but evidence would need to be repeated clinically for CBD to become an accepted therapy for diabetic retinopathy
Edema also occurs in the body’s extremities and results in swollen ankles, legs, and feet in people with diabetes. This may sometimes be accompanied by diabetic foot ulcers which occur in 15% of all people with diabetes and precede 84% of diabetic lower leg amputations6 (Brem, H. & Tomic-canic, M, 2007).
CBD extracts have been clinically effective in treating intractable neurogenic pain34 (Wade, D. T. et al., 2003) and for treating pain in disorders such as multiple sclerosis, cancer, and other chronic pain conditions35 (Urits, I. et al., 2019).
CBD and Cardiomyopathy
Diabetics were found to be out of a prospective study of 5000 people, 2 and 5 times more likely to develop heart failure in men and women respectively36 (Wang, J. et al., 2006). Cardiovascular death accounts for 75% of all deaths in people with diabetes37 (Selvin, E. et al., 2004)
Diabetic heart abnormalities include decreased diastolic compliance and left ventricular hypertrophy. The underlying factor for these abnormalities includes interstitial fibrosis and myocyte hypertrophy as well as contractile protein glycosylation36 (Wang, J. et al., 2006). Diabetic cardiomyopathy is marked by oxidative stress and an increase in pro-inflammatory cytokines.
CBD attenuated myocardial dysfunction, cardiac fibrosis, oxidative/ nitrative stress, inflammation, cell death, and interrelated signaling pathways in mice38 (Rajesh, M. et al., 2010). CBD signaling from acute and prolonged exposure enhances vasorelaxation39 (Stanley, C. P., Hind, W. H. & O’Sullivan, S. E., 2013) and maybe a potential therapeutic for cardiovascular disease.
Conclusion
As Cannabis legalization becomes more globally prevalent, more clinical research will become accessible. The potential complications of diabetes mellitus may be intimidating, but CBD may be able to relieve some of the physical and biochemical stress leading to a better quality of life.
Cannabis has upwards of 140 unique cannabinoids with some minor ones such as THCV, CBC, CBN, and CBG having potential therapeutic effects. Extracts contain a variety of terpenoids and phenolic compounds that may enhance the action of cannabinoids at their targets40 (Russo, E. B., 2011). The future will likely see the emergence of CBD-dominant plant extracts which include these minor cannabinoids and terpenes.
Disclaimer
There has been plenty of research in the field of Cannabis science and CBD as a potential therapeutic. However, CBD should not supplement nor supersede physician medical advice. Diabetics number one priority is to live a healthy lifestyle and maintain target hemoglobin A1c levels. Epidiolex® has been approved by the FDA as an antiepileptic drug and so far, has not been approved for diabetes. CBD is non-toxic and can be tolerated at high doses12 (World Health Organization) but CBD with THC will cause a ‘high’ feeling. CBD is considered a dietary supplement or natural health product (NHP) in the USA and therefore does not require FDA regulation. It is important to read and follow the label before use of any CBD product.
References
1Zhang, X. F. & Tan, B. K. H. Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 28, S37–S42 (2000).
2Wang, X. et al. Identification of a Molecular Signature in Human Type 1 Diabetes Mellitus Using Serum and Functional Genomics. J. Immunol. 180, 1929–1937 (2008).
3Kahn, B. B. & Flier, J. S. Obesity and insulin resistance. J. Clin. Invest. 106, 473–481 (2000).
4Leiter, E. H. The genetics of diabetes susceptibility in mice. FASEB J. 3, 2231–2241 (1989).
5Nathan, D. M. et al. Modern-day clinical course of type 1 diabetes mellitus after 30 years’ duration: The diabetes control and complications trial/epidemiology of diabetes interventions and complications and Pittsburgh epidemiology of diabetes complications experience (1983-2. Arch. Intern. Med. 169, 1307–1316 (2009).
6Brem, H. & Tomic-canic, M. Cellular and molecular basis of wound healing in diabetes Find the latest version : Cellular and molecular basis of wound healing in diabetes. 117, 1219–1222 (2007).
7Pisanti, S. et al. Cannabidiol: State of the art and new challenges for therapeutic applications. Pharmacol. Ther. 175, 133–150 (2017).
8Booz, G. W. Cannabidiol as an emergent therapeutic strategy for lessening the impact of inflammation on oxidative stress. Free Radic. Biol. Med. 51, 1054–1061 (2011).
9Pertwee, R. G. The diverse CB 1 and CB 2 receptor pharmacology of three plant cannabinoids: Δ 9-tetrahydrocannabinol, cannabidiol and Δ 9-tetrahydrocannabivarin. Br. J. Pharmacol. 153, 199–215 (2008).
10Laprairie, R. B., Bagher, A. M., Kelly, M. E. M. & Denovan-Wright, E. M. Cannabidiol is a negative allosteric modulator of the cannabinoid CB1 receptor. Br. J. Pharmacol. 172, 4790–4805 (2015).
11Campos, A. C., Moreira, F. A., Gomes, F. V., del Bel, E. A. & Guimarães, F. S. Multiple mechanisms involved in the large-spectrum therapeutic potential of cannabidiol in psychiatric disorders. Philos. Trans. R. Soc. B Biol. Sci. 367, 3364–3378 (2012).
12World Health Organization. Department of Essential Medicines and Health Products, Team of Innovation, A. and U. Cannabidiol (CBD) Critical Review Report. Expert Comm. Drug Depend. 4–7 (2018).
13Small, E. & Beckstead, H. . Common Cannabinoid Phenotypes in 350 stocks of Cannibis. AGRIS 144-165e (1973).
14Stott, C. G., White, L., Wright, S., Wilbraham, D. & Guy, G. W. A phase i study to assess the single and multiple dose pharmacokinetics of THC/CBD oromucosal spray. Eur. J. Clin. Pharmacol. 69, 1135–1147 (2013).
15Lucas, C. J., Galettis, P. & Schneider, J. The pharmacokinetics and the pharmacodynamics of cannabinoids. Br. J. Clin. Pharmacol. 84, 2477–2482 (2018).
16Tham, M. et al. Allosteric and orthosteric pharmacology of cannabidiol and cannabidiol-dimethylheptyl at the type 1 and type 2 cannabinoid receptors. (2019). doi:10.1111/bph.14440
17Castillo, A., Tolón, M. R., Fernández-Ruiz, J., Romero, J. & Martinez-Orgado, J. The neuroprotective effect of cannabidiol in an in vitro model of newborn hypoxic-ischemic brain damage in mice is mediated by CB2 and adenosine receptors. Neurobiol. Dis. 37, 434–440 (2010).
18Iannotti, F. A. et al. Nonpsychotropic plant cannabinoids, Cannabidivarin (CBDV) and Cannabidiol (CBD), activate and desensitize Transient Receptor Potential Vanilloid 1 (TRPV1) channels in vitro: Potential for the treatment of neuronal hyperexcitability. ACS Chem. Neurosci. 5, 1131–1141 (2014).
19Deutsch, D. G. & Chin, S. A. Enzymatic synthesis and degradation of anandamide, a cannabinoid receptor agonist. Biochem. Pharmacol. 46, 791–796 (1993).
20Laprairie, R. B., Bagher, A. M. & Denovan-wright, E. M. Cannabinoid receptor ligand bias : implications in the central nervous system. Curr. Opin. Pharmacol. 32, 32–43 (2017).
21El-Remessy, A. B. et al. Neuroprotective effects of cannabidiol in endotoxin-induced uveitis: Critical role of p38 MAPK activation. Mol. Vis. 14, 2190–2203 (2008).
22Hua, T. et al. Crystal Structure of the Human Cannabinoid Receptor CB 1. Cell 167, 750-762.e14 (2016).
23Morales, P., Goya, P. & Jagerovic, N. Emerging strategies targeting CB2 cannabinoid receptor: Biased agonism and allosterism. Biochem. Pharmacol. 157, 8–17 (2018).
24Navarro, G. et al. Targeting cannabinoid CB2 receptors in the central nervous system. Medicinal chemistry approaches with focus on neurodegenerative disorders. Front. Neurosci. 10, 1–11 (2016).
25Ruhaak, L. R. R. et al. Evaluation of the Cyclooxygenase Inhibiting Effects of Six Major Cannabinoids Isolated from Cannabis sativa. 34, 774–778 (2011).
26Costa, B. et al. Oral anti-inflammatory activity of cannabidiol, a non-psychoactive constituent of cannabis, in acute carrageenan-induced inflammation in the rat paw. Naunyn. Schmiedebergs. Arch. Pharmacol. 369, 294–299 (2004).
27Ribeiro, A. et al. Cannabidiol, a non-psychotropic plant-derived cannabinoid, decreases inflammation in a murine model of acute lung injury: Role for the adenosine A2A receptor. Eur. J. Pharmacol. 678, 78–85 (2012).
28Weiss, L. et al. Cannabidiol lowers incidence of diabetes in non-obese diabetic mice. Autoimmunity 39, 143–151 (2006).
29Weiss, L. et al. Cannabidiol arrests onset of autoimmune diabetes in NOD mice. Neuropharmacology 54, 244–249 (2008).
30Klein, B. E. K., Moss, S. E., Klein, R. & Surawicz, T. S. The Wisconsin Epidemiologic Study of Diabetic Retinopathy. Ophthalmology 98, 1261–1265 (1991).
31Trap-Jensen, J. & Lassen, N. A. Increased capillary diffusion capacity for small ions in skeletal muscle in long-term diabetics. Scand. J. Clin. Lab. Invest. 21, 116–122 (1968).
32Porta, M., Selva, M. La, Molinatti, P. & Molinatti, G. M. Endothelial cell function in diabetic microangiopathy. Diabetologia 601–609 (1987).
33Rajesh, M. et al. Cannabidiol attenuates high glucose-induced endothelial cell inflammatory response and barrier disruption. Am. J. Physiol. – Hear. Circ. Physiol. 293, 610–619 (2007).
34Wade, D. T., Robson, P., House, H., Makela, P. & Aram, J. A preliminary controlled study to determine whether whole-plant cannabis extracts can improve intractable neurogenic symptoms. Clin. Rehabil. 17, 21–29 (2003).
35Urits, I. et al. An Update of Current Cannabis-Based Pharmaceuticals in Pain Medicine. Pain Ther. 8, 41–51 (2019).
36Wang, J., Song, Y., Wang, Q., Kralik, P. M. & Epstein, P. N. Causes and Characteristics of Diabetic Cardiomyopathy. Rev. Diabet. Stud. 3, 108–108 (2006).
37Selvin, E., Marinopoulos, S., Berkenblit, G., Rami, T. & Brancati, F. L. Meta-Analysis: Glycosylated Hemoglobin and Cardiovascular Disease in Diabetes Mellitus. (2004).
38Rajesh, M. et al. Cannabidiol attenuates cardiac dysfunction, oxidative stress, fibrosis, and inflammatory and cell death signaling pathways in diabetic cardiomyopathy. J. Am. Coll. Cardiol. 56, 2115–2125 (2010).
39Stanley, C. P., Hind, W. H. & O’Sullivan, S. E. Is the cardiovascular system a therapeutic target for cannabidiol? Br. J. Clin. Pharmacol. 75, 313–322 (2013).
40Russo, E. B. Taming THC: Potential cannabis synergy and phytocannabinoid-terpenoid entourage effects. Br. J. Pharmacol. 163, 1344–1364 (2011).