Arthritis is a challenging diagnosis to live with at any age, but it can be especially difficult for seniors. Not only does the stiffness and pain make it hard to get around, but the worry of a flare-up is always on your mind. As a result, using CBD for arthritis in seniors seems to be an effective approach to managing this discomfort. People even report using cannabis oil for rheumatoid arthritis that’s rich in CBD. In fact, of all age groups that cover CBD use, ages 60 and older is the most widely reported.
As we age, our bodies go through many changes—one of the most common changes in the development of arthritis. Arthritis usually comes along with chronic pain, and is a frustrating condition that can make it very challenging to do the things we love. While there are many options to help relieve pain from arthritis, it never hurts to explore new ways to treat arthritis that are emerging as science evolves. This is where CBD for arthritis comes in to play.
Enjoying your reading so far? Sign up to become part of the NPB community and receive a free eBook, 20% off your next order, and access to ton of educational information about cannabinoids like CBD and Delta 8. NPB hosts, arguably, the largest collection of cannabinoid info on the internet. There is no better place to learn than our educational databse.


CBD and Arthritis Pain in Seniors
CBD is medical cannabis that is used to treat various health conditions. CBD is short for cannabidiol, and is one of the many compounds found in medical marijuana products and hemp-derived items alike. CBD, unlike THC, has no intoxicating effects, though. As a result, it will not make you high.
Related read: CBD for Seniors
However, CBD is effective in treating various medical conditions. One of these medical conditions is the pain of arthritis in seniors. A medical review conducted in 2016 showed that CBD products effectively reduced arthritis pain and inflammation. Most people who deal with arthritis know that arthritis related pain can be crippling, so this comes as outstanding news.
Another medical review conducted in 2017 showed that CBD effectively treated other medical conditions such as anxiety, depression, and chronic pain. While more research needs to be done on the effects of CBD products on arthritis pain, the current evidence suggests that a CBD treatment is an effective option for arthritis care.
Different Types of Arthritis
Osteoarthritis is the most prevalent form of arthritis. When knee cartilage begins to break down, this is known as osteoarthritis. Because this cartilage protects your bones from friction, it may cause discomfort and joint pain, and even joint damage. Inflammation can result as a consequence of this condition. In addition, because cartilage decays at a slower rate than other parts of the body, osteoarthritis is a degenerative disease.
Another type of arthritis that develops in seniors is Rheumatoid arthritis. This condition is when the immune system attacks the lining of the joints and can cause inflammation, swelling, and chronic pain. Rheumatoid arthritis can also lead to joint damage and deformity.
Osteoarthritis
Discover: CBD Oil for Osteoarthritis
Osteoarthritis is the most common type of arthritis, affecting around 27 million Americans. It occurs when the cartilage between the joints breaks down, causing the bones to rub against each other. This can lead to pain, stiffness, and inflammation.
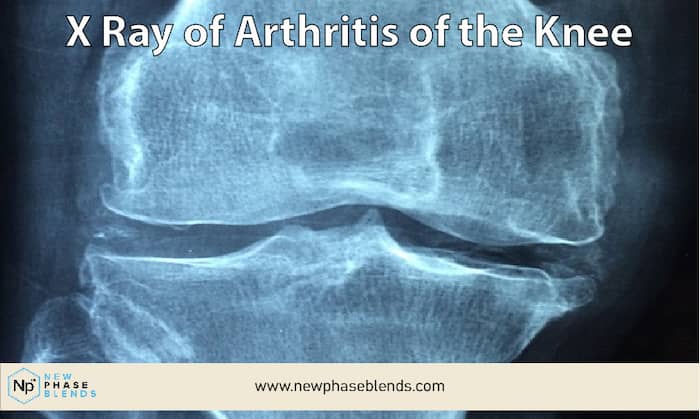
The best arthritis creams can do a very effective job and helping people deal with the pain associated with this type of arthritis. Osteoarthritis is more common than another type of arthritis known as Rheumatoid arthritis.
Applying a transdermal cannabidiol reduces inflammation, which can do wonders for your arthritis pain.
Rheumatoid Arthritis
Rheumatoid arthritis is a less common but more serious type of arthritis. It occurs when the body’s immune system attacks the joints, causing inflammation.
This can damage the cartilage and bone, leading to pain, swelling, and deformity.
Rheumatoid arthritis can cause more than joint pain, though. According to the Mayo Clinic, “In some people, the condition of Rheumatoid arthritis can damage a wide variety of body systems, including the skin, eyes, lungs, heart and blood vessels.”
Cannabis Oil for Rheumatoid Arthritis Pain
Thankfully, you can use cannabis oil for rheumatoid arthritis pain relief. In fact, a vast majority of people that use cannabis oil for rheumatoid arthritis report a very noticeable pain relief.
This is most likely because of the effects of CBD on arthritis. Sure, CBD can be used for several different reasons, but using it for inflammation and associated inflammatory pain seems to be the most popular reason for use. The arthritis foundation has listed substantial evidence in using things like CBD oil for rheumatoid arthritis relief.
If you haven’t tried any yet, I highly recommend you do.
Type: Pure CBD Oil
CBD: 33mg or 66mg per serving
Features: Broad or full spectrum, premium CBD oil
We use a CBD rich cannabis extract. Our cannabis oil can be purchased with 0.0% THC, or 0.3% THC. Regardless it will not get you high. Not everyone who uses a CBD treatment to relieve pain wants to get high – that’s why we made ours with this formulation.
Also, if you don’t like it, just return it. We’ll give you all of your money back. We only want you to pay if you’re truly happy with your results.
How CBD Help Relieve Arthritis Symptoms
CBD oil is known to possess pain-relieving and anti-inflammatory properties. CBD oil interacts with receptors in the body’s endocannabinoid system, which is why a CBD treatment can be such a life-changing experience. Pain receptors respond to CBD use, too.
Related: How CBD Works in Your Body
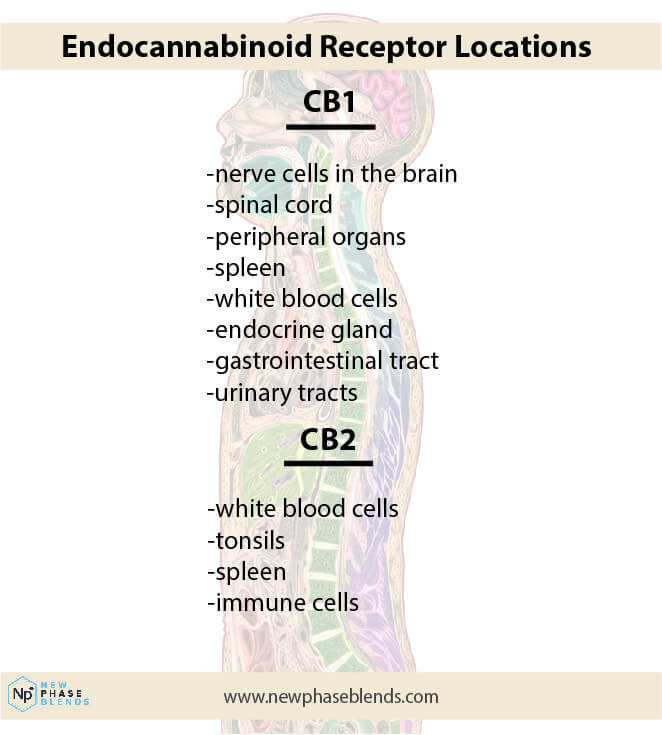
CBD oils are generally considered safe, but they can cause side effects such as drowsiness, dry mouth, and diarrhea when taking too much. CBD oils should also not be used with some other medications. Speak to a doctor before using CBD oil if you are on a medication regimen.
They will know better than any online website whether or not what you are taking will interact with cannabidiol (CBD).
CBD Products Made to Help Chronic Pain From Arthritis
CBD Products for Sale by New Phase Blends
Type: CBD oil for energy
CBD: 16mg per serving
Features: Synephrine and CBD blend for energy
Type: CBD Acne Cream
CBD: 1000mg per 1oz jar
Features: Salicylic acid and CBD blend to stop acne
Type: High strength CBD balm
CBD: 500mg, 1000mg, or 2000mg
Features: Full spectrum, lavender scented
Type: CBD Starter Kit Bundle
Includes: Tincture, Balm, and Gummies
Features: You create your own kit with your custom product choices
Type: Pure CBD Softgel Capsules
CBD: 40mg per capsule
Features: Broad spectrum, vegan certified softgels
Type: Pure CBD Gummies
CBD: 45mg per gummy
Features: Full spectrum, premium quality CBD gummies
Type: Pure CBD Oil
CBD: 33mg or 66mg per serving
Features: Broad or full spectrum, premium CBD oil
CBD: 45mg per gummy
Features: Patent-pending CBD and melatonin formula for sleep
Type: CBD oil for sleep
CBD: 66mg per serving
Features: Patent-pending CBD and melatonin formula for sleep
CBD stands for cannabidiol, a natural ingredient found in hemp plants. It’s one of the numerous chemicals (called cannabinoids) that people are currently researching. CBD has been praised for its promise as a healing remedy for various diseases, including arthritis.
CBD, unlike cannabis, has no psychoactive effects so you won’t experience a “high.” As a result, researchers investigated how CBD might be utilized therapeutically.
Discover: CBD Cream for Back Pain
CBD product distributors sell a wide range of CBD products, including:
Oils and Tinctures – CBD extract is suspended in a carrier oil consumed orally through this method. There are three types of CBD oil spectrums include: isolate, full-spectrum CBD, and broad-spectrum CBD.
Edibles – CBD edibles in the form of gummies, chocolates, beverages, and other items are available.
Topicals – CBD cream, salves, and balms may be applied to the skin directly to treat chronic pain. Many people prefer this form for joint pain.
Transdermal Patches – Patches work similarly to topicals, except they stick to your skin and penetrate it more effectively.
Vaporizers – Some people, on the other hand, prefer to use CBD inhalants for quicker results.
Using CBD For Arthritis
CBD is a natural anti-inflammatory that can help to reduce pain and stiffness from chronic inflammation. Additionally, CBD effectively reduces anxiety, which can help manage the stress of living with arthritis that many seniors have. For seniors, using CBD for arthritis may offer a welcome relief from the challenges arthritis can bring.
Because CBD’s legal position is so complicated on the federal level, it’s still tough to obtain research funding. Nevertheless, early studies, anecdotal evidence, and high-scoring consumer testimonies point to CBD’s curative properties.
Discover: How CBD Works in the Body
CBD reduced pain in rats with arthritis in one study. Another study has confirmed that CBD reduces inflammation by suppressing the body’s natural immune response. You’ll also discover a lot of consumer feedback and success stories online that support these findings.
A CBD transdermal gel was utilized in the research on CBD’s impact on arthritis. This delivery method is one of the finest choices for CBD for arthritis for a few reasons.
Benefits of CBD For Arthritis in Seniors
Medical cannabis is becoming increasingly popular to manage various health conditions. CBD, or cannabidiol, is one of the active ingredients in medical cannabis. Recent studies have shown that 42 percent of baby boomers are already using full-spectrum CBD to help with joint and knee pain relief. On top of this, many healthcare providers now recommend using CBD for inflammatory pain.
In animal research, CBD has been shown to have antioxidant, pain and inflammation relieving properties. Therefore, by taking CBD, you may be able to reduce the signs and symptoms of arthritis. However, it should be emphasized that CBD does not cure arthritis.
It’s crucial to talk with your doctor first if you’re thinking of using medical cannabis to manage your arthritis symptoms because medical cannabis has not yet been clinically evaluated for the treatment of arthritis discomfort.
Chronic Pain Suppression
According to a medically reviewed study, 62.2 percent of marijuana users took the cannabis plant for chronic pain relief. CBD, short for cannabidiol, is derived from the cannabis plant. It is one of many compounds found in the plant, and it does not have the psychoactive effects that THC does.
Related: Taking CBD for Muscle Pain
Taking CBD can help to alleviate pain by interacting with receptors in the brain and body. It can also help to reduce inflammation and improve sleep. In addition, CBD may help to lower blood pressure. When choosing how much of a CBD product to use for arthritis, start with a small dose and gradually increase as needed.
Using something like CBD gummies for pain relief is a very popular way to help with this sort of discomfort. Have back pain? Take a gummy, or another type of CBD product that you enjoy, and see just how well it will work for you.
Nerve Protectant
Nerve pain is a severe ailment that might make it difficult or impossible to carry out everyday activities. Cannabis plant extracts with CBD can also protect your nerves, which is interesting since it has been shown to reduce joint nerve pain. In addition, it aids in the relief of joint neuropathy. As a result, it’s useful for diseases such as arthritis, cancer, and multiple sclerosis.
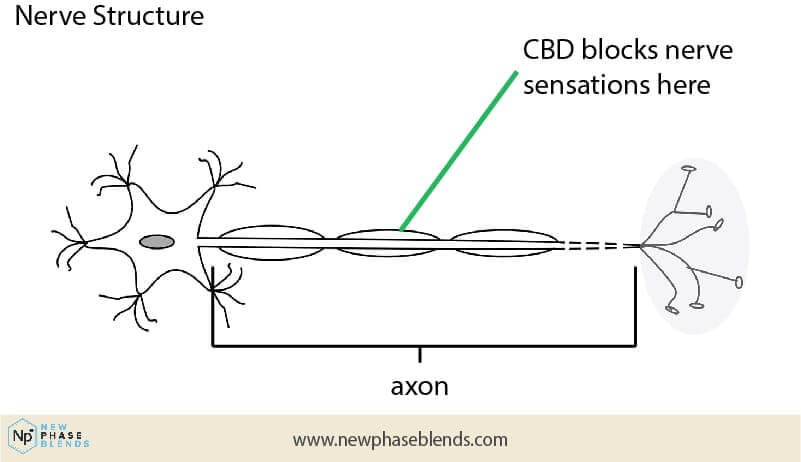
CBD is found in cannabis plants, and the organic hemp plant is incredibly high in CBD content. Hemp-derived CBD products are a powerful and safe treatment for nerve pain and nerve injury, and they may be used alone or in combination with other pain and inflammation treatment. Taking CBD oil really helps people in this area.
Joint Support
CBD is effective in reducing inflammation, which can help relieve the pain of arthritis. A medically reviewed CBD product that contains pure CBD and is free of impurities can be an effective way to reduce inflammation.
CBD products containing coconut oil can help further reduce inflammation and improve joint function. If you are considering taking CBD for joint support, be sure to consult with your physician first.
The Best CBD for Arthritis in Seniors
CBD Products for Sale by New Phase Blends
Type: CBD oil for energy
CBD: 16mg per serving
Features: Synephrine and CBD blend for energy
Type: CBD Acne Cream
CBD: 1000mg per 1oz jar
Features: Salicylic acid and CBD blend to stop acne
Type: High strength CBD balm
CBD: 500mg, 1000mg, or 2000mg
Features: Full spectrum, lavender scented
Type: CBD Starter Kit Bundle
Includes: Tincture, Balm, and Gummies
Features: You create your own kit with your custom product choices
Type: Pure CBD Softgel Capsules
CBD: 40mg per capsule
Features: Broad spectrum, vegan certified softgels
Type: Pure CBD Gummies
CBD: 45mg per gummy
Features: Full spectrum, premium quality CBD gummies
Type: Pure CBD Oil
CBD: 33mg or 66mg per serving
Features: Broad or full spectrum, premium CBD oil
CBD: 45mg per gummy
Features: Patent-pending CBD and melatonin formula for sleep
Type: CBD oil for sleep
CBD: 66mg per serving
Features: Patent-pending CBD and melatonin formula for sleep
Depending on why you’re using CBD, different form factors exist. If you’re buying a high potency CBD oil, you should notice results no matter which forms you take. Transdermal CBD patches, on the other hand, appear to be the best option for arthritis in older people. With all the medically reviewed information the arthritis society now approves of using approved nonprescription CBD products to relieve arthritis pain.
CBD Topical Balms
CBD balms or creams applied topically, unlike transdermal patches, do not enter the circulation. Instead, they function by stimulating the endocannabinoid system (ECS) in your skin. The ECS in our skin is responsible for sweating, hair growth, and immunity response.
Transdermal CBD Patches
Our skin’s primary purpose is to serve as a protective barrier. It prevents anything from coming into the body. That includes the CBD that is meant to help. Transdermal gel employs chemical boosters that allow active substances to enter the circulation to get through it.
These chemicals are non-toxic and safe to use as directed, even though they enable nicotine patches, hormonal therapies, and contraceptives to enter the skin.
Transdermal CBD patches may also provide several more advantages over simply allowing them to permeate the skin.
CBD Creams Are Best
Before investing in a more expensive product, test the waters. A CBD topical does not function in the same way as transdermal patches. Although you may feel better effects than a patch, you will notice more minor changes.
CBD creams are an inexpensive, safe approach to experimenting with how much CBD to use and observing how your body responds.
Discover: Hemp CBD Balm
CBD products may be used in a variety of different ways. CBD topicals come in a variety of packaging and sizes, so you can carry them with you wherever you go. You may use it whenever and wherever you need it, and you’re done in less than a minute.
Once a CBD transdermal patch is applied, it stays in place for an extended period. So you’ll have to use it as directed for up to 72 hours to get the most out of all of the CBD inside.
Improve your skin’s health. Many CBD topicals include additional botanicals, essential oils, olive oil, and natural chemicals beneficial to your skin. Transdermal patches target specific areas of the body rather than our epidermis (outer layer of skin).
CBD creams and CBD lotion are designed to improve the condition of your skin while also making it look and feel fabulous.
CBD Oils and Tinctures
The most frequent variety of CBD is typically CBD oils, tinctures, and extracts. There are a few distinctions between the three on a technical level. But don’t worry too much about that.
Discover: How to Use CBD Oil For Pain
The terms “CBD oil” and “tincture” mean the same thing and are used interchangeably.
CBD oil is usually taken sublingually. You place the drops under your tongue, and hold there for about 1 – 2 minutes. You can go ahead and swallow the rest. CBD does wonders for things like pain and nerve damage, as you have probably gathered by now
You may also eat CBD oil or add it to food and beverages if you don’t like the hemp taste. However, because CBD is digested, its efficacy will decline. There are seemingly limitless possibilities. Because this is the most popular style, you’ll have hundreds of excellent choices.
CBD oils come in a variety of strengths and flavors and a wide range of botanicals, or simply as raw hemp extract with no additives. You can discover a CBD oil formulated specifically for the condition you want help with if you do some research.

Other Benefits of CBD for the Elderly
CBD has a lot of other advantages that make it an excellent addition to any wellness regimen. There is more to CBD than inflammatory arthritis and joint pain relief. The elderly especially stand to gain from CBD’s potential health benefits. Take a look at just a few of them below.
Reduction of Internal Inflammation
Cannabidiol (CBD) has been shown to have an anti-inflammatory effect. One of CBD’s most researched applications is its ability to combat inflammation. CBD’s anti-inflammatory qualities may assist elders in a variety of ways.
CBD topicals will likely help with pain caused by arthritis by lowering inflammation indirectly. So, too, CBD is said to help treat inflammatory bowel diseases such as IBS.
Get Better Sleep
According to research, CBD helps people with insomnia sleep better. Patients reported longer, uninterrupted sleep than the placebo group. These effects varied but persisted for months after the study ended. More restful sleep means more energy, enhanced brain function, and a greater sense of well-being for seniors.
Related read: Using CBD for Insomnia
Relieve Anxiety
A study conducted in 2019 evaluated the effectiveness of CBD in treating anxiety. As a result, patients’ anxiety levels fell by an astounding 80% during the first month of treatment, according to the same study.
These reduced anxiety levels were persistent throughout the trial duration. In addition, a 2015 research discovered that CBD reduced anxiety symptoms in a wide range of illnesses. However, exactly how CBD for anxiety works is still unknown.
Common Questions About CBD Use and Arthritis
Is CBD Oil Good For Arthritis?
CBD oil can be an effective treatment for both osteoarthritis and rheumatoid arthritis. It helps to reduce pain and inflammation and has been shown to be more effective than traditional medications.
But there’s one thing you need to keep in mind – there are more than 100 types of arthritis. Most of the differences are minor, but one thing seems to be kept in common among all of these different forms: inflammation.
Discover: Compare Nordic Oil CBD With New Phase Blends
Have you ever noticed that most arthritis medications are some sort of anti-inflammatory? Well, it is because the inflammation of the joints causes most of the symptoms people feel when they struggle with arthritis. In fact, arthritis is more of a widely-used term that describes inflammation in the joints.
Is CBD Legal?
Is CBD Legal?
The legality of CBD in the US was recently in dispute. Some states have legalized medical and recreational marijuana, but marijuana is still classified as a Schedule I narcotic under federal law. Because CBD is produced from the cannabis plant, it was assumed to be illegal. This is no longer the case. Everyone can now enjoy the health effects of CBD, legally.
The 2018 Farm Bill has since passed. CBD has been removed from the federal controlled substances act, which one caveat to the farmers.
While farmers may cultivate hemp and CBD, they are not permitted to develop THC. Hemp may now be grown legally, but there is a limit on the amount of THC allowed.
Is CBD Safe to Use?
While it sounds fantastic, is CBD safe?
In general, CBD is considered to be non-toxic and safe in both liquid or topical form. It has a shallow danger profile. There has never been a case of CBD toxicity reported. However, some users may feel drowsy after using CBD, so you should keep this in mind if you intend on working heavy equipment or driving.
Do CBD Gummies Help With Arthritis
CBD gummies can help with arthritis pain, similar to how other forms of CBD products work. The one downside about using gummies is their kick-in time is a bit longer (30 mins to 1.5 hours).
Summary - Seniors Using CBD For Arthritis Relief
There are the minor annoyances of old age: wrinkles, pains, sores, and other symptoms. Many health problems have been more prevalent among the elderly population. When it comes to managing the issues connected to aging, CBD has shown itself to be a safe and natural alternative to prescription medications.
Arthritis is on of the several painful conditions that many people suffer from, and it can be incredibly annoying to live with. Thankfully, CBD oil has been shown to be an effective, natural treatment for arthritis symptoms, as it helps to reduce pain and inflammation.
Before using any CBD oil product for pain management, you should speak with your healthcare provider and do some research on the brands you buy – it’s worth the time. While we prefer you purchase your CBD from us, there are several other phenomenal brands you might prefer – and that’s okay!